This post is part of a series of quarterly roundups on scientific integrity.
The second quarter of 2021 featured an impressive increase in COVID-19 vaccinations accompanied by concerns that federal agencies aren’t doing enough to support other preventive measures—which are likely to be more necessary as the delta variant of the virus spreads. Proponents of evidence-based policy expressed alarm at FDA’s approval of an Alzheimer’s drug not proven to substantially improve symptoms, and support for processes designed to safeguard scientific integrity in the federal government.
Emphasizing vaccination above other protections
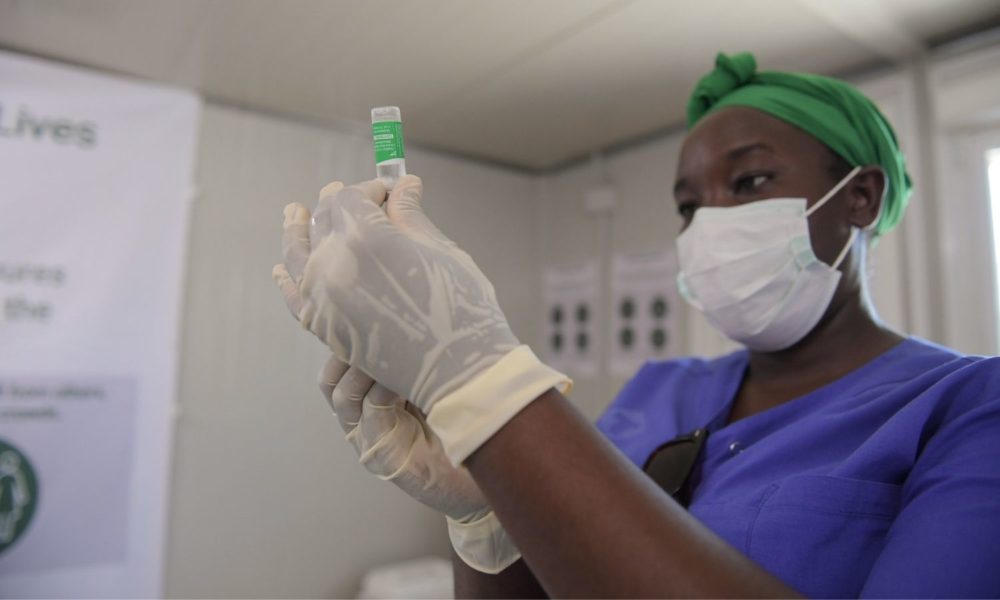
By the end of June, the US had gotten at least one COVID-19 vaccination to 65% of adults, and children as young as 12 started getting shots after FDA authorized the Pfizer vaccine for this age group in May. This increase in vaccinations has helped reduce the spread of COVID-19 and limited illness severity in vaccinated people who contract the virus, and it is a tremendous achievement from both the scientists behind the vaccine and the teams who help bring it to the public. However, racial and ethnic inequities in vaccination rates remain (although they have narrowed) in the US and at the global level, and many US workers still lack the paid leave that would allow them to get their shots and recover from any side effects without risking their jobs or financial stability. More work is necessary to both improve access and overcome hesitancy and misperceptions. The global spread of the delta variant, which can infect people with less exposure, makes the vaccination task even more urgent.
Vaccination can’t be the only response to COVID-19, though. In addition to the problems of inequitable distribution, vaccines still aren’t authorized for children under 12, and many with compromised immune systems remain susceptible to severe COVID-19 even if they get the shots. No vaccine is 100% effective, and even these remarkably effective COVID-19 vaccines might be less protective against future variants—which will continue to emerge as long as global vaccine distribution is limited in countries with fewer resources and uptake remains patchy in even a well-resourced nation like the US. Combining vaccination with preventive steps like masking and ventilation is the most effective way to limit the spread of this disease.
Given the evidence about who’s been vaccinated and how the virus spreads, it’s hard to understand how CDC could take the actions that it has over the past few months. In early May, many public health advocates were relieved when the agency finally acknowledged the role of aerosol transmission—if disappointed that CDC didn’t take the obvious next step of making recommendations for better ventilation. So it was a shock when on May 13, the agency abruptly altered its guidance for vaccinated people to advise that those who are fully vaccinated no longer need to wear masks in most indoor settings (with exceptions for spaces like healthcare facilities and public transit). The agency based this advice primarily on several studies indicating that fully vaccinated people are at low risk of developing symptomatic COVID-19 and spreading the disease to others. In an extensive critique of CDC’s guidance, National Nurses United points out that a large proportion of the studies CDC cites are preprints that haven’t yet gone through a journal’s peer-review process, and that some of the studies are funded by vaccine manufacturers. They also stress the fact that multiple layers of protection are still advisable, especially in order to protect nurses and others who are at greater risk.
The fact that CDC seems to treat this as a narrow question of vaccine effectiveness rather than a larger question about how best to equitably protect public health is troubling. Engaging in more consultation with social scientists, instead of focusing so heavily on papers about post-vaccination infection rates, might have helped the agency realize that the response to their guidance would be for states and employers to drop their mask requirements without any kind of mechanism for ensuring that only the fully vaccinated were going mask-free—and indeed, mask mandates fell immediately in several states. More discussion with equity experts might have resulted in CDC advising localities and organizations to maintain mask requirements until vaccination rates for Black and Latinx people matched those of the White population. It’s not clear that CDC adequately considered these forms of evidence, though. Instead, they turned from a focus on communities to a focus on individuals, telling people “your health is in your hands,” and they appear to have abandoned the central public health tenet of protecting and promoting the health of all people. COVID-19 cases have since increased in areas where vaccination rates are low.
CDC’s downplaying of the need for protections other than vaccines seems to have played a role in weakening the ability of the Occupational Safety and Health Administration (OSHA) to protect workers. One of President Biden’s first executive orders instructed OSHA to consider issuing an emergency temporary standard to protect workers from COVID-19. The agency sent the White House a draft standard that applied across industries—but the emergency standard released on June 10 applies only to healthcare settings. It requires employers to develop and implement coronavirus safety policies, ensure employees are wearing masks, maintain physical distance, and screen employees for COVID-19. Although these are welcome steps, limiting them to healthcare employers leaves out many other essential workers, including those in meatpacking, agriculture, food service, retail, transportation, warehouses, childcare, and hospitality—industries where workers are disproportionately likely to be Black and Latinx. In order to issue a standard that applied to these workers, OSHA would have had to show that they remain in grave danger. CDC’s failure to acknowledge that these workers remain at elevated risk even when many are vaccinated makes it much harder for OSHA to defend a multi-industry rule against inevitable court challenges.
Looking ahead: On June 25, 2021, the World Health Organization urged fully vaccinated individuals to continue wearing masks in indoor settings. The CDC now suggests that fully vaccinated people should continue to wear masks if they live in high-transmission areas.
FDA approves Alzheimer’s drug with insufficient evidence and against expert advice
Members of FDA’s scientific advisory committee voted overwhelmingly against approving Biogen’s Alzheimer’s drug Aduhelm (aducanumab) because they did not find that the company’s trials provided convincing evidence that the drug slowed cognitive decline—though they did find a risk of serious side effects like brain swelling and bleeding. FDA’s decision to approve the drug anyway was so shocking that three advisory committee members resigned in protest.
FDA decided to approve the drug not because patients in the trials experienced cognitive improvements, but because patients in one of the two trials exhibited reductions in the beta amyloid plaque that builds up in the brains of Alzheimer’s patients. However, as National Center for Health Research authors noted in the medical journal BMJ, other drugs that have been found to reduce beta amyloid have failed to achieve cognitive improvements in clinical trials. In addition, FDA approved Aduhelm for all Alzheimer’s patients, even though clinical trials enrolled only participants with mild disease and their demographics did not reflect those of US Alzheimer’s patients.
“If expert advice is ignored when making drug approval decisions, what is the point of establishing these committees?” asked UCS Senior Analyst Genna Reed. “And what does it say to the public that the FDA isn’t making its decision using expert advice? Can the public fully trust that FDA is making decisions based on the science and not on pressure it’s getting from pharmaceutical companies with massive financial stakes in gaining its approval?”
Looking ahead: The chairs of the House Committees on Oversight and Reform and on Energy and Commerce announced that their committees will investigate the Aduhelm approval.
Improving scientific integrity infrastructure
It’s clear that even with a president who has expressed a strong commitment to scientific integrity, more safeguards are needed to ensure that agencies consider evidence and expert advice appropriately when making policy decisions. Fortunately, efforts are underway to improve the scientific integrity infrastructure.
In a process President Biden set forth during his first week in office, a Scientific Integrity Task Force composed of high-level staff from a range of agencies has established working groups to examine instances in which scientific integrity policies were not followed or enforced, and to identify effective practices for ensuring integrity, bolstering research transparency, and protecting science communication. To inform the work of the Task Force, the White House Office of Science and Technology Policy (OSTP) has requested comments from the public on the following: (1) The effectiveness of federal scientific integrity policies and needed areas of improvement; (2) good practices federal agencies could adopt to improve scientific integrity; and (3) other topics or concerns that federal scientific integrity policies should address.
To develop stronger policies, it can be helpful to consider instances where current policies failed to prevent interference. EPA is one agency that has begun correcting the scientific record damaged under the Trump administration, though some worry that the agency might not go far enough to hold wrongdoers accountable. Non-governmental organizations are also looking to past problems to inform future solutions: Climate Science Legal Defense Fund and the Government Accountability Project (with the American Geophysical Union, Environmental Data & Governance Initiative, Jacobs Institute of Women’s Health, and Union of Concerned Scientists as advisory partners) have teamed up to launch the Scientific Integrity Reporting Project, an initiative aimed at documenting past and ongoing threats to scientific integrity to ensure that science can contribute to evidence-based policymaking without the influence of partisan politics. Federal employees, grantees, and contractors who experienced or witnessed interference can report their experiences through secure and confidential channels.
Looking ahead: There is no deadline for contacting the Scientific Integrity Reporting Project.
Pieces on the Biden Administration’s First 100 Days:
Biden’s first 100 days: Where he stands on science
Biden Has Reversed Trump’s War on Science in His First 100 Days
The First 100 Days of the Biden-Harris Administration: Reproductive Rights, Health and Justice
100 Days in Independent Agency Nominations
Also:
Over 260 groups call on Biden to improve whistleblower protections
EPA scraps Trump rule that weakened air pollution regulations
Minority representation in US science workforce sees few gains
Senate confirms Eric Lander to lead White House science shop
The State of Independent Agency Nominations – Update for Spring 2021
U.S. Interior Dept revokes Trump policies, puts climate at center of decisions
New Resources:
Equity Forward resource: Biden Administration Timeline: Science and Evidence Guiding Policy and Funding
Open the Government resource: Progress Tracker
Union of Concerned Scientists resource: How Is President Biden Doing on Science and Democracy? Tracking Progress on Science in Decisionmaking Under the Biden Administration